Fertility treatment is booming, and IVF clinics say the pandemic is driving more people through their doors.
Fertility treatment is booming. IVF clinics say the pandemic is driving more people through their doors enquiring about egg freezing and treatments to have a baby.
Independent data backs this up. The Victorian Assisted Reproductive Treatment Authority’s 2021 annual report reveals a 20% surge in the number of people receiving treatment in Victoria last year, and a 27% jump in cycles. So, more women are having more cycles.
So, what should your patients know about fertility preservation and treatment when they ask you for a referral? Here are three things you can tell them to help manage their expectations and prepare them for what’s to come.
Age is the biggest factor
While IVF has helped millions of people around the world have children, about half of those who try IVF don’t take home a baby. And few have a baby after one cycle of IVF, especially if they’re in their late 30s or older.
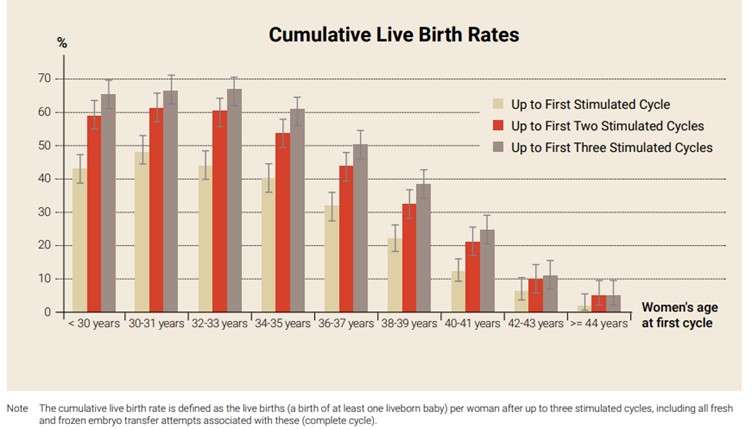
The age of a woman when she freezes her eggs or starts IVF treatment is the biggest contributor to her chance of success. This is demonstrated clearly in the graph below. It shows the cumulative chance of a baby after one, two and three IVF cycles for women, depending on their age at the start of treatment. Each cycle includes any frozen embryos that are used to attempt a pregnancy.
It shows that, for women aged up to 30 years, the average chance of a baby was 43% after one stimulated cycle and 66% after three stimulated cycles. For women aged 42–43, the chance of a baby was 6% after one and 11% after three stimulated cycles.
Almost one-quarter of women who have IVF are aged 40 years or older. They invest a lot of time and money for a minuscule chance of having a baby. For women in this age group, using donor eggs from a younger woman might be a better option.
It could take time and significant investment
The other take- away from this graph is that IVF usually takes more than a few months and can sometimes take years. For most people, the ultimate chance of having a baby increases for each additional cycle, up until five cycles.
So, it’s helpful to have a series of treatments in mind rather than expecting immediate success when embarking on IVF. That way, expectations may be more realistic, and people may be more likely to try again if treatment fails.
This can help with budgeting, too. People can expect to pay up to $5000 in out-of-pocket costs for each cycle after Medicare rebates are applied.
IVF with the lot may not be worth it
One of the things that makes fertility treatment challenging for some people is the growing number of options available on top of standard IVF. Many of these extras are not proven to improve the chance of a baby or will help only some people.
For example, many clinics now use a special technique created to overcome male infertility for people without sperm problems, even though it doesn’t improve the chance of a live birth for them. The technique, known as intracytoplasmic sperm injection, or ICSI, is now the main fertilisation method used in Australia, even when sperm counts are normal.
ICSI adds around $500 in out-of- pocket costs for patients. In Victoria, around 75% of cycles used ICSI in 2020-21. This is despite only 30% of couples having male infertility and 15% severe male infertility.
Another expensive addition to IVF is genetic testing of embryos, which costs about $700 per embryo. Pre-implantation genetic testing for aneuploidy (chromosome abnormalities), known as PGT-A, is an “add on” used to help choose embryos with the right number of chromosomes. It’s promoted by IVF clinics as a way to increase the chance of success, especially for women over 35. But the evidence shows that, in most cases, PGT-A doesn’t improve the chance of a baby.
So, if you are referring a patient to start fertility treatment, it’s a great time to promote the Choosing Wisely questions below, with an extra question relevant to IVF: Will this increase my chance of a baby? It might help your patients save time and money that could be better spent on evidence-based treatment in their quest for a child.
- Do I really need this test?
- What are the risks?
- What are the costs?
- Are there simpler, safer options?
- What happens if I don’t use it?
For independent information about fertility treatment, visit the Victorian Assisted Reproductive Treatment Authority’s website. For more evidence-based information about factors that affect fertility, visit the Your Fertility website.
This article first appeared on healthed.com.au


