GPs should take up the rebate on offer from November. Here are some questions to ask.
Almost 300 people are diagnosed with diabetes in Australia each day.
We are talking about 1.8 million Australians living with the condition, and the majority of those have a regular GP. On average, a GP might have 70 to 80 patients with type 2 diabetes in their caseload.
Diabetes is a chronic illness, meaning there is a timeline and a continuum of involvement in patient care, not only at diagnosis but also supporting them throughout their life living with diabetes. Chronic illnesses require clinical systems to support a patient because they often involve timely changes in lifestyle and medication choices as the condition evolves or complications emerge.
Patient-centric management of people with diabetes means creating shared health goals, such as individualised haemoglobin A1c (HbA1c) levels. Having regular HbA1c assessments allows healthcare providers to advise people on their risks of current and future complications.
Federal Minister for Health Greg Hunt announced in March that $2.1 million would be allocated to the reimbursement of routine HbA1c point-of-care tests for people with diagnosed diabetes from 1 November.
This is a wonderful step from the government to support quality care in general practice, as it cements the importance of primary care in managing people with diabetes. The reimbursement allows both practices and patients to have a choice when it comes to HbA1c testing, as the additional value of point-of-care testing (PoCT) becomes more accessible. Any investment that improves the systems supporting people with diabetes and emphasises the central role of general practices as being hubs for diabetes is a great thing.
Patients have lives, and they are busy, so engaging someone to have regular appointments and meet their goals such as HbA1c can be a challenge. People come to the clinic, and they may forget to get things done and not had a pathology test review. If a test is available when a person attends a GP appointment, we can give timely feedback without having the patient return later.
Point-of-care testing is particularly helpful when monitoring patients at difficult points in their lives, such as those who are a bit overwhelmed by their condition. This model of care does not replace traditional pathology investigation; it adds a safety net. People who have not kept up with regular blood testing can be identified and supported when they come into the practice.
In addition, it rounds out the care service for those who have had problems with adherence to important diabetes-specific goals.
Point-of-care analysers generally require a drop of blood from a finger prick or small urine sample to produce results. The technology has been advancing for the past 10 years, with some of the available systems being the size of a toaster and portable.
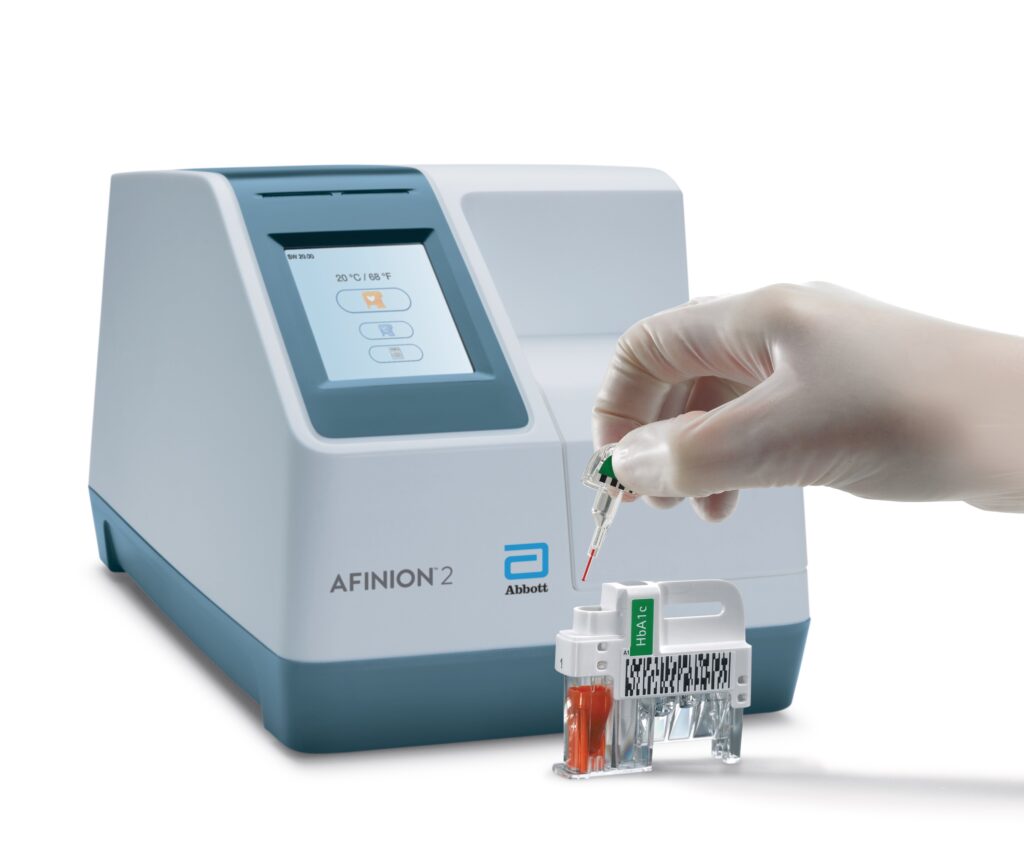
One of the biggest misconceptions is that PoCT results are not as accurate as formal pathology testing. This is incorrect: some point-of-care systems, such as the Afinion 2 Analyzer, have been proven to be highly accurate in several studies. Accuracy and precision for this specific system is on par with laboratory testing for HbA1c diagnosis. These analysers have been independently assessed, and the government has decided to follow that up by appropriate reimbursement.
It is important that GP clinics seize this opportunity for improved clinical diabetes care and make use of the reimbursement. Uptake of PoCT will not only benefit patients and practices, but could also help to expand the reimbursement criteria to other assays and conditions in the long term.
Some of the currently available analysers can process additional assays on top of HbA1c for diagnosis and monitoring of diabetes, including lipid panels and ACR testing that is so important for a diabetes annual cycle of care. C-reactive protein (CRP) assays can be conducted with some systems, which may aid with the appropriate prescribing of antibiotics.
The acquisition of a point-of-care analyser therefore provides a range of services which go beyond what was previously on offer for patients and elevates the level of general practice care services. The RACGP has developed quality standards for PoCT which are comprehensive and support practices integrating this technology into care.
If you plan to make the most of the reimbursement and offer PoCT at your clinic, here are some important considerations. First, does the manufacturer of the point-of-care analyser provide support and training for practice staff? Second, is the analyser accredited, and does it meet the Medicare Benefits Schedule reimbursement requirements? Third, can the information provided be easily incorporated in medical records? And finally, can the chosen analyser be expandable to other metabolic testing when appropriate?
Collectively, all GPs need to be educated about the availability of the technology and the reimbursement to encourage them to utilise this in an effective and timely way. Point-of-care testing allows the provision of pathology services within the clinic, eliminating the extra step where some patients fall by the wayside.
PoCT will enhance the quality of care for patients in regional and rural Australia, where access to pathology laboratories may be geographically difficult. In addition, this technology may assist adherence to agreed pathology testing intervals at practices that support patients with specific needs, including cross-cultural and other linguistically diverse groups or people with mental health disorders.
Finally, any general practices that want to invest in enhancing the quality of their care services to people with diabetes can now consider PoCT as a realistic option.
Dr Gary Deed is a general practitioner with a specific interest in diabetes and is the current chair of the diabetes specific interest network of the Royal Australian College of General Practitioners.