What began as a simple system has grown so many tentacles it’s effectively impossible to understand and comply with.
In 1975 when Medibank (later Medicare) was first introduced, the regulatory landscape was pretty simple.
Forty-five years later, it has morphed into a twisted and snarled morass of incoherent laws and other legal instruments, so complex and mercurial it would be beyond the comprehension of anyone.
The original Medicare scheme was built on strong constitutional foundations. It comprised little more than an important new Act of Parliament, the Health Insurance Act 1973 (Cwth), plus a few additional elements that doctors were required to navigate, such as various contracts, worker’s compensation arrangements, and a new policing system called the Medical Services Committees of Inquiry. A lot has changed, mostly in the past 20 years.
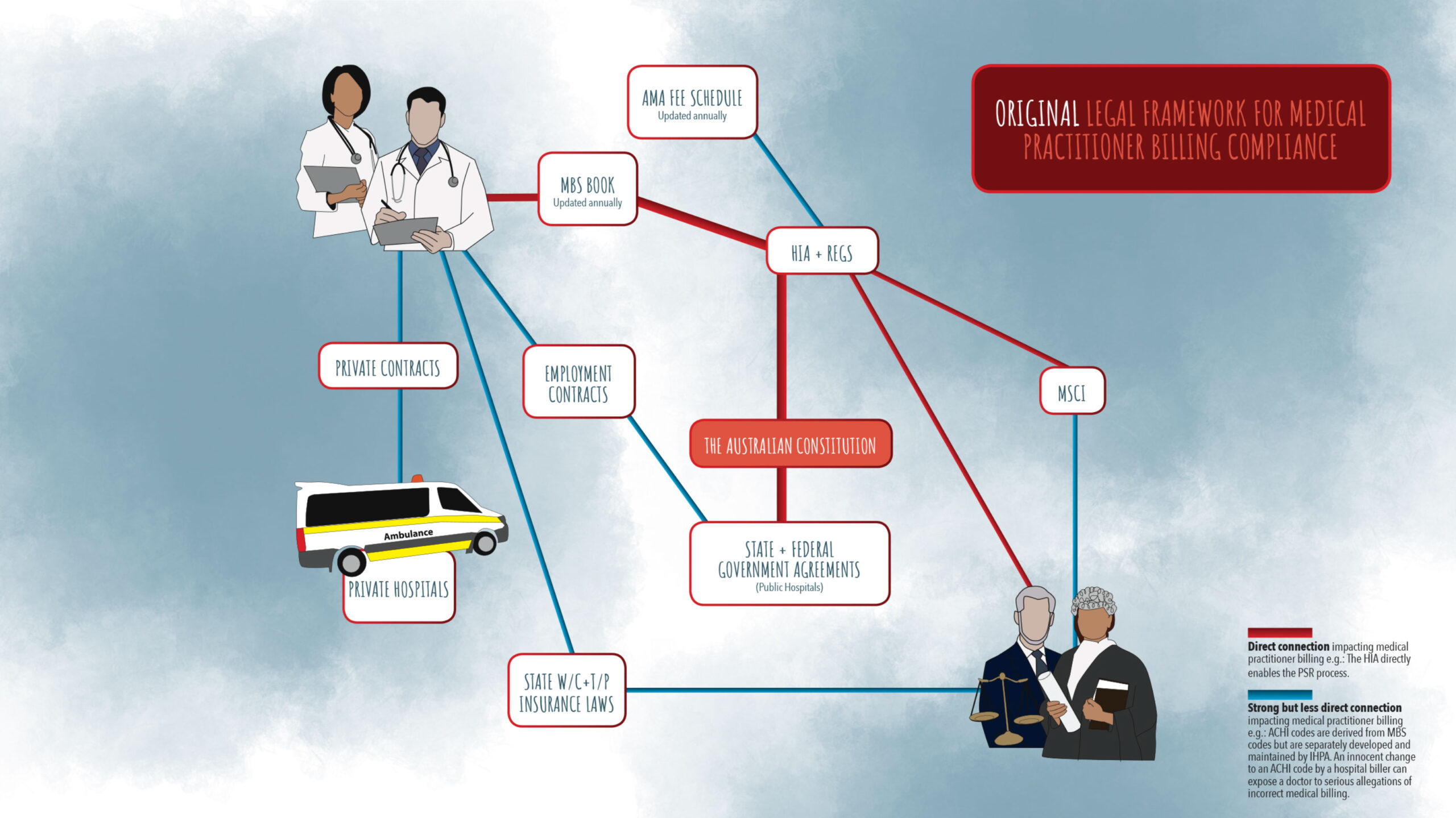
The way laws intersect, overlap, and sometimes disagree, interests legal academics. My Medicare PhD was positioned largely through a legal lens because I had found myself referencing these laws daily as part of my job. One day, after going through all the historical data and in order to clear my mind, I drew the original medical billing compliance framework on a whiteboard. It was pretty straightforward.
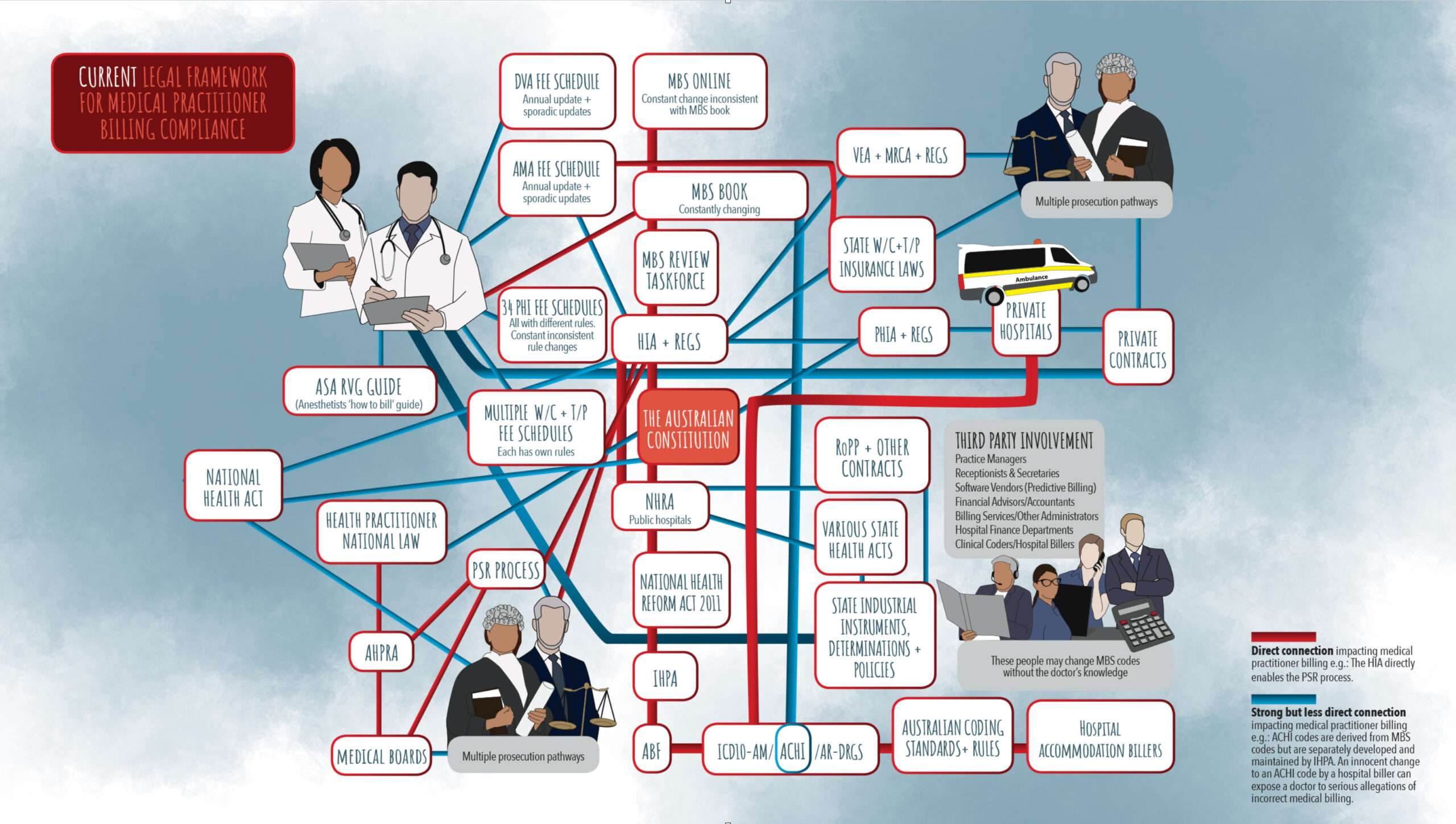
Further along my doctoral journey, I stood in front of the same whiteboard, but this time I drew the connections between every law and each legal instrument that I am required to reference and use every day at work, and I ended up with this … sobering.
I have conservatively estimated that this regulatory gordian knot, of important medical billing laws and critical rules that doctors are expected to know, or be familiar with, would extrapolate out to well over 20,000 pages.
By comparison, a key business law, the Corporations Act 2001 (Cwth), with a relatively modest 3,000-plus pages, has been declared so prolix and incomprehensible by the legal profession, that it is currently undergoing a 10-year law reform process.
But it doesn’t stop there: in 2020 alone, 255 statutory instruments were added to the Federal Register of Legislation with the words “Health Insurance” in the title, and only 53 of those were covid-19 related. Therefore 202 statutory instruments relating to “Health Insurance” were enacted in one year alone, all of which impacted medical billing compliance in some way.
So, of course compliance is impossible.
Even if you can find the law that applies to particular conduct, it is often incomprehensible. And a system this shambolic is very vulnerable to misuse, both deliberate and unintentional. There are regulatory gaps everywhere.
Attempts to address compliance problems have been clumsy and unsuccessful. This is largely because, in the same way that having a bit of a crack at cardiac surgery is unlikely to go well without having a deep understanding of human anatomy and physiology, having a crack at reforming health system law will also go badly without understanding the operation of the system in its entirety.
I will never forget the day when a furious hospital client yelled at me, demanding to know what on earth we thought we were doing changing an MBS item number allocated by a surgeon. We administered the accommodation coding and billing for that client not the medical billing – who knew those things were even interrelated? So, when the subsequent root cause analysis investigation revealed we had made an innocent error caused by mismatched ACHI (Australian Classification of Health Interventions) and MBS codes, I began to understand just how far the ripples travel, when changes are made to a part of our health system by people who do not understand, or have to administer, the operation of the whole.
The one common thread in this labyrinth is the ubiquitous MBS, our list of trusty item numbers. It is everywhere, in every nook and cranny of the health system. The MBS is the start point of every clinical encounter in this country, and the first code allocated to kick off a patient journey. Everything is connected to it, whether directly or indirectly – the AMA codes, Workcover billing rules, ACHI codes, the National Health Reform Agreement, everything.
So, as our bedrock dataset, central to the operation of the entire health system, the MBS needs to be gracefully integrated into Australia’s overarching digital health strategy.
Having focused on the current distress and confused tangle that is our current national universal healthcare system, Medicare, in forthcoming articles I will outline how we could disentangle it and achieve comparative order and clarity.
It will take a village, but what a relief it would be for patients, providers, payers, and administrators if it looked more like this:
Margaret Faux is a health system administrator, lawyer and registered nurse with a PhD in Medicare compliance, and is the CEO of AIMAC, which offers courses and explainers on legally correct Medicare billing