Around one in five individuals with COVID-19 may experience venous or arterial thromboemboli, which significantly increase the odds of death.
Welcome to The Medical Republic’s COVID Catch-Up.
It’s the day’s COVID-19 news in one convenient post. Email bianca@biancanogrady.com with any tips, comments or feedback.
24 November
- Thromboembolic events affect one in five with COVID-19, and are linked to higher mortality.
- Contact tracing error in the UK may have led to additional 125,000 cases and 1500 deaths.
- Randomised controlled trial finds no benefit from convalescent plasma.
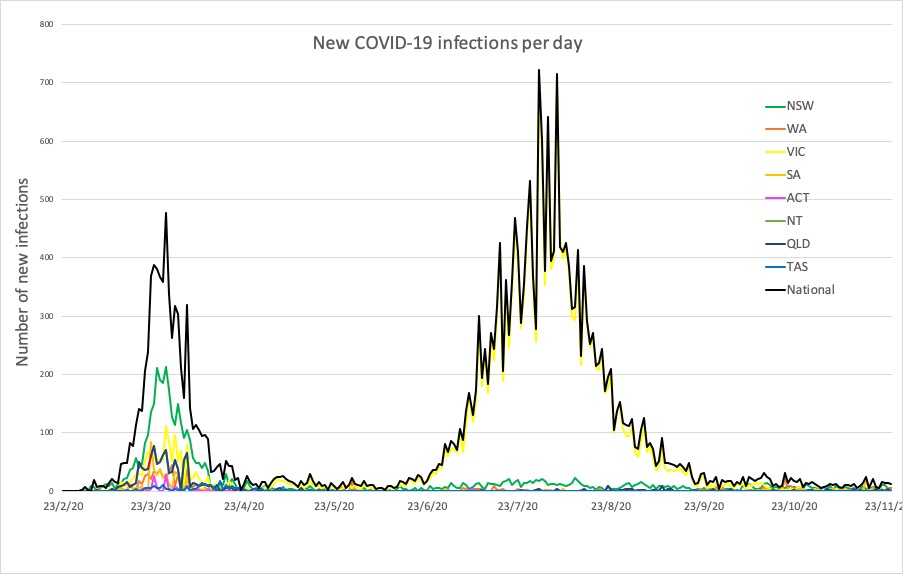
- Latest confirmed COVID-19 infection numbers from around Australia.
- Around one in five individuals with COVID-19 may experience thromboembolic events, and these significantly increase the odds of death, a systematic review and meta-analysis has found.
A paper published in EClinical Medicine reported the analysis of 42 studies of venous and arterial thromboembolism among patients with COVID-19.
Among the 16 studies of venous thromboembolism, the overall rate of VTE was 21% among patients not in intensive care but as high as 31% among intensive care patients, which the authors noted was significantly higher than what is seen in patients hospitalised with other acute infections.
The 28 studies of deep venous thrombosis reported an overall rate of 20%, and the overall rate of pulmonary embolism in the 31 studies of that outcome was 7% in non-intensive care, 19% in intensive care, and 22% in postmortem studies.
The overall pooled mortality rate in all patients who experienced thromboembolic events was 23%, compared to 13% in patients without thromboemboli, representing a 74% higher odds of death. - Even the smallest delays in implementing contact tracing of COVID-19 cases can have devastating consequences.
Between September 25 and October 2, a data processing error in the UK delayed the referral of nearly 16,000 COVID-19 cases – around 15%-20% of cases – to the contact tracing system. The error resulted from the fact that the Excel spreadsheet format used to record cases had 65,536 row-limit, so the additional case information was truncated.
A report on that incident has now estimated it may have contributed to more than 125,000 additional infections and 1500 additional COVID-19 deaths.
The non-peer-reviewed report by researchers at the University of Warwick and Harvard Business School used the fact that the glitch affected different parts of the UK with differing intensities to extrapolate the effects. They saw ‘strongly accelerated growth’ in the numbers of positive cases around the time of the misreporting, followed by persistently higher case numbers, “indicating that the data glitch propelled England to a different stage of pandemic spread.”
“The gist of our main findings squares with the previous state of evidence: despite numerous challenges faced by a contact tracing system such as a population’s potential lack of trust, non-adherence and privacy concerns, this non-pharmaceutical intervention can have a strong impact on the progression of an infectious disease,” the authors wrote. - A randomised, placebo-controlled trial of convalescent plasma for severe COVID-19 pneumonia has found no evidence of improved clinical outcomes from the treatment.
Writing in the New England Journal of Medicine, researchers reported the outcomes of a study in which 228 patients were assigned to receive high-titre convalescent plasma and 105 to receive placebo. They found no difference between the treatment and placebo groups in clinical status at 30 days, nor in the secondary outcomes of 30-day mortality or time to hospital discharge.
“This finding is in contrast to the findings of a series of nonrandomized studies claiming convalescent plasma to be of substantial benefit and illustrates the importance of randomized, controlled trials, especially in the context of a pandemic,” the authors wrote. - Here are the latest confirmed COVID-19 infection numbers from around Australia to 9pm Tuesday:
National – 27,848 with 907 deaths
ACT – 115 (0)
NSW – 4548 (6)
NT – 47 (0)
QLD – 1197 (1)
SA – 558 (2)
TAS – 230 (0)
VIC – 20,345 (0)
WA – 808 (4)