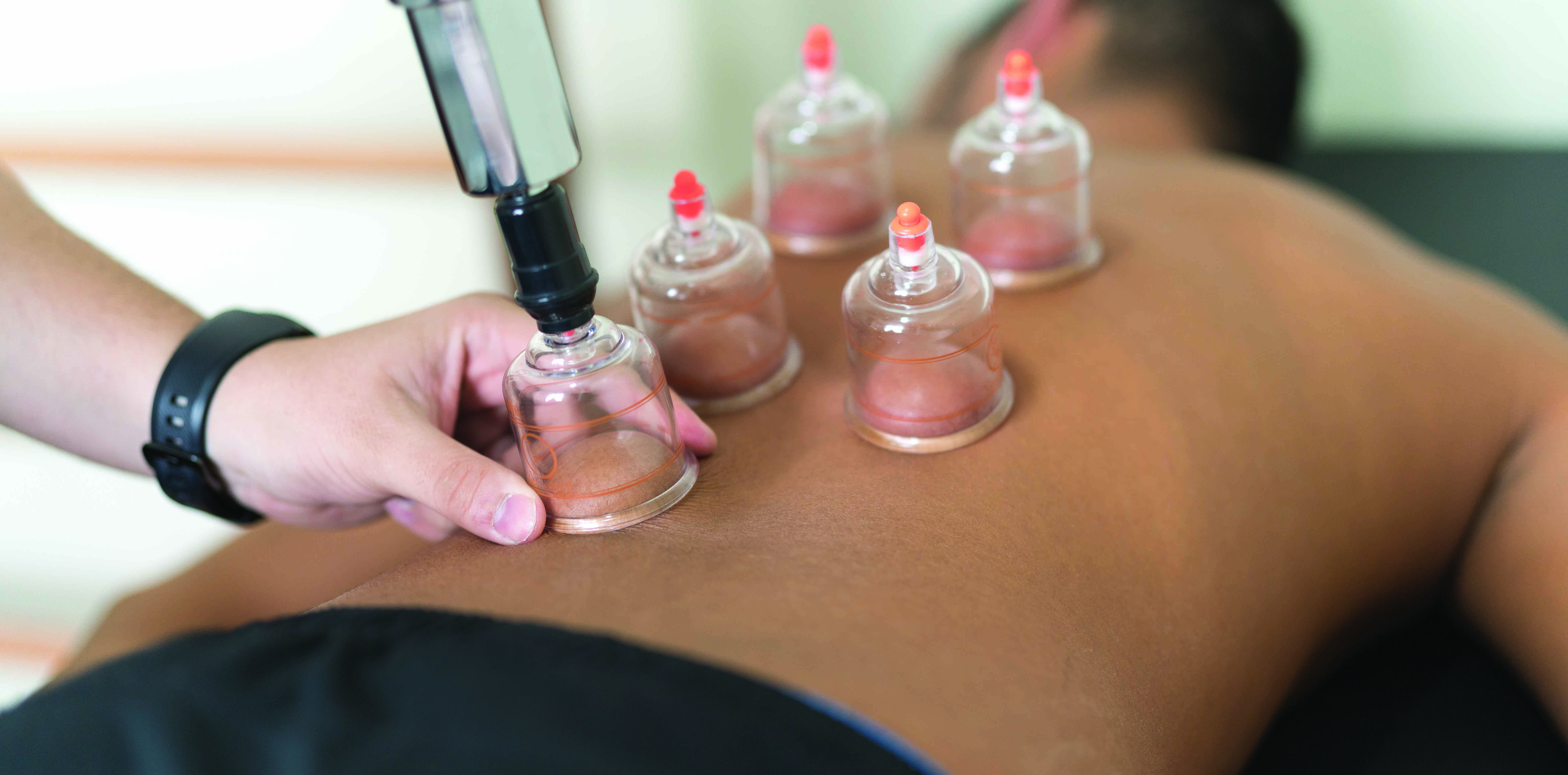
Not everyone is happy with the the Medical Board’s draft guidelines for regulating medical practitioners who practise unconventional medicine
The Medical Board of Australia is asking for feedback on its first-ever draft guidelines for regulating medical practitioners who practise unconventional medicine.
The board launched the public consultation in response to growing concerns around unethical behaviour by health practitioners operating outside the bounds of conventional medicine.
In the absence of regulation, some vulnerable patients were falling prey to medical practitioners, perhaps with commercial conflicts of interest who were failing to gain informed consent, using treatments with no evidence base, and prescribing inappropriate medications, the Medical Board said.
The draft guidelines encompassed a lot of different areas – including integrative medicine, complementary or alternative medicine, unconventional medicine and emerging treatments.
It ran the full gamut from alternative medicines with no proven efficacy (including homeopathy) to controversial therapies (such as long-term antibiotics for Lyme-like disease, experimental stem cell therapies, and minerals, supplements and hormones in the absence of a therapeutic need).
The board said these guidelines were not set in stone, and invited debate from stakeholders. The Board proposed two, broad options: 1) keeping with the status quo; and 2) strengthening the current guidance by explicitly outlining the Board’s expectations.
The draft guidelines listed key principles, such as asking your patient about their use of complementary medicine regardless of whether you recommended these treatments, and informing your patients that there was limited reputable scientific evidence for the use of some of these therapies.
Doctors also had a duty to warn patients about the potential harms, including financial costs, of pursuing unconventional treatments, while respecting their patient’s right to make informed decisions about their health, the board said.
“Always act honestly and only in your patient’s best interests,” the board advised. “Do not discourage the use of conventional treatment options when this is clinically inappropriate.”
With more than two-thirds of consumers using complementary medicines, it was important that every practitioner be aware of this area of practice, the board said.
“We are ready to work with the Medical Board of Australia on this,” Dr Penny Caldicott, a GP and the President Australasian Integrative Medicine Association, said.
“We are a bit concerned about integrative medicine being put into this bigger group. We know that the medicine that we do is low risk, very comprehensive and of significant benefit to our patients.”
GPs who practise integrative medicine generally take a more holistic approach to patient care through longer consultations and more crossing over into alternative and complementary medicine.
“To practise integrative medicine, you have to first and foremost be a very good conventional medical practitioner,” Dr Caldicott said.
Although some GPs were a bit nervous about dabbling in unconventional medicine, the field was growing in popularity. The RACGP’s special interest group in integrative medicine now had around 700-800 GP members, Dr Caldicott said.
Integrative medicine doctors were seeing more young people with unexplained symptoms, such as trouble sleeping, fatigue, anxiety or depression and short-term memory problems – and they found that following traditional guidelines was sometimes not enough to help these patients.
“Integrative medicine helps us to have other approaches, once we have done all the things that we would do medically,” Dr Caldicott said.
Dr Caldicott said there were also concerns about integrative medical doctors being too heavily scrutinised by regulators. This was a feeling mirrored in conventional general practice, where AHPRA has come under fire for doggedly pursuing vexatious complaints, and putting innocent GPs under unfair amounts of stress and scrutiny.
Falling on the other end of the spectrum, Associate Professor Ken Harvey, the president of Friends of Science in Medicine, called the board’s draft guidelines “wishy-washy” and said he would be pushing for a total clampdown on useless medicine.
“The boards have been very reluctant [to regulate],” he said. “They bullshit on about, ‘Oh, we might be stifling innovation’. Well, you are not stifling innovation by banning homeopathy. And you are not stifling innovation by encouraging people to do controlled clinical trials.”
“It’s a positive move to put it up for public consultation. But in my opinion the draft paper … doesn’t grapple with the real issues.”